Share:
On November 1, 2022, the Centers for Medicare and Medicaid Services (CMS) issued the Calendar Year (CY) 2023 Physician Fee Schedule (PFS) final rule. The rule updates payment rates and finalize policy changes effective January 1, 2023. See the Press Release, Fact Sheet, Fact Sheet (MSSP), and the Final Rule.
General
CMS finalized its proposal to add some services to the Medicare Telehealth Services List on a Category 3 basis through the end of 2023, some of which had not been previously added to the Medicare Telehealth List during the PHE, but will be added on a sub regulatory basis.
In addition, CMS finalized its proposal that Medicare telehealth services furnished on or before the 151st day after the end of the PHE, in alignment with the extensions of telehealth-related flexibilities in the CAA, 2022, will continue to be processed for payment as Medicare telehealth claims when accompanied with the modifier “95”. CMS also finalized its proposal that physicians and practitioners can continue to report the place of service code that would have been reported had the service been furnished in-person during the 151-day period after the end of the PHE, as finalized on an interim basis in the March 31 IFC.
Payment for Medicare Telehealth Services Under Section 1834(m) of the Act
Requests to Add Services to the Medicare Telehealth Services List for CY 2023
CMS found that none of the requests received by the February 10 submission deadline met Category 1 or Category 2 criteria for permanent addition to the Medicare telehealth services list. As a reminder, Category 1 are services that are similar to professional consultations, office visits, and office psychiatry services that are currently on the Medicare Telehealth Services list, and the criterion for adding services under Category 2 is that there is evidence of clinical benefit if provided as telehealth.
CMS also assessed the appropriateness of adding the proposed services to the Medicare Telehealth Services List on a Category 3 basis instead. CMS did not propose changes to the length of time the services included on the temporary Category 3 basis. Category 3 will continue to be included through the end of CY 2023. In the event the public health emergency (PHE) extends into CY 2023, CMS may consider revising this policy.
After consideration of public comments, CMS is finalizing the proposed addition of CPT codes 90901, 97150, 97530, 97537, 97542, 97763, and 98960-98962 to the Medicare Telehealth Services List on a Category 3 basis through the end of CY 2023. CMS believes their proposal, consistent with the amendments made by provisions of the CAA, 2022, to extend the period that these services will be available on the Medicare Telehealth Services List temporarily for the PHE by 151 days following the end of the PHE will further enhance the opportunity for the collection of information on the experiences of clinicians who are furnishing telehealth services during the PHE for COVID–19. This will also help CMS to determine which services may ultimately be eligible for permanent addition under Category 1 or Category 2 criteria. CMS encourages interested parties to use this extended time period to gather data on use of services, that is more than statements of support and more than subjective attestations of clinical benefit, to support their potential addition in future rulemaking.
CMS did not finalize its proposal to keep telephone E/M services on the Medicare Telehealth Services List after the end of the PHE and the 151-day post-PHE extension period. CMS believes the statute requires that telehealth services be so analogous to in-person care such that the telehealth service is essentially a substitute for a face-to-face encounter. CMS does not believe that, outside of the circumstances of the PHE, the telephone E/M services would be analogous to in-person care; nor would they be a substitute for a face-to-face encounter. While CMS acknowledges that audio-only technology can be used to furnish mental health telehealth services to patients in their homes under certain circumstances after the PHE ends, two-way, audio-video communications technology continues to be the appropriate standard that will apply for Medicare telehealth services after the PHE and the 151-day extension period. At the conclusion of the PHE and the 151-day extension period provided by the CAA, 2022, the only Medicare telehealth services that will be permitted to be furnished using audio-only technology will be the mental health telehealth services. When a practitioner furnishes such an E/M service using audio-only technology, they would bill for the same service they would bill if the service had been furnished in person. As such, there is not a need to add the telephone-only E/M codes to the Medicare Telehealth Services List for this purpose.
CMS did not finalize its proposal to add GI Tract Imaging, CPT code 91110 and Ambulatory Continuous Glucose Monitoring, CPT code 95251 services to the Medicare Telehealth Services List on a Category 3 basis. CMS does not believe these CPT codes describe services that are a substitute for an in-person visit, and the services that are not inherently face-to-face services are not services that can be furnished as Medicare telehealth services.
CMS finalized its proposal to add CPT codes 95970, 95983, and 95984 to the Medicare Telehealth Services List on a Category 3 basis. Medicare claims data suggest that these services are being provided via telehealth and CMS believes there is some possible clinical benefit for these services when furnished via telehealth; however, there is not yet sufficient evidence available to consider the services for permanent addition to the Medicare Telehealth Services List under the Category 1 or Category 2 criteria.
CMS finalized its proposal to retain emotional/behavior assessment, psychological, or neuropsychological testing and evaluation services on the Medicare Telehealth Services List on a Category 3 basis. CMS believes more time may be necessary to develop evidence that could support the decision to add these services to the Medicare Telehealth Services List permanently on a Category 1 or Category 2 basis.
Other Services Proposed for Addition to the Medicare Telehealth Services List
CMS finalized its proposal to add a number of services to the list on a Category 3 basis that are currently included on the Medicare Telehealth Services List temporarily during the PHE. These services would be included on the Medicare Telehealth Services List through 2023 to allow us to evaluate data that may support their permanent addition to the list on a Category 1 or Category 2 basis.
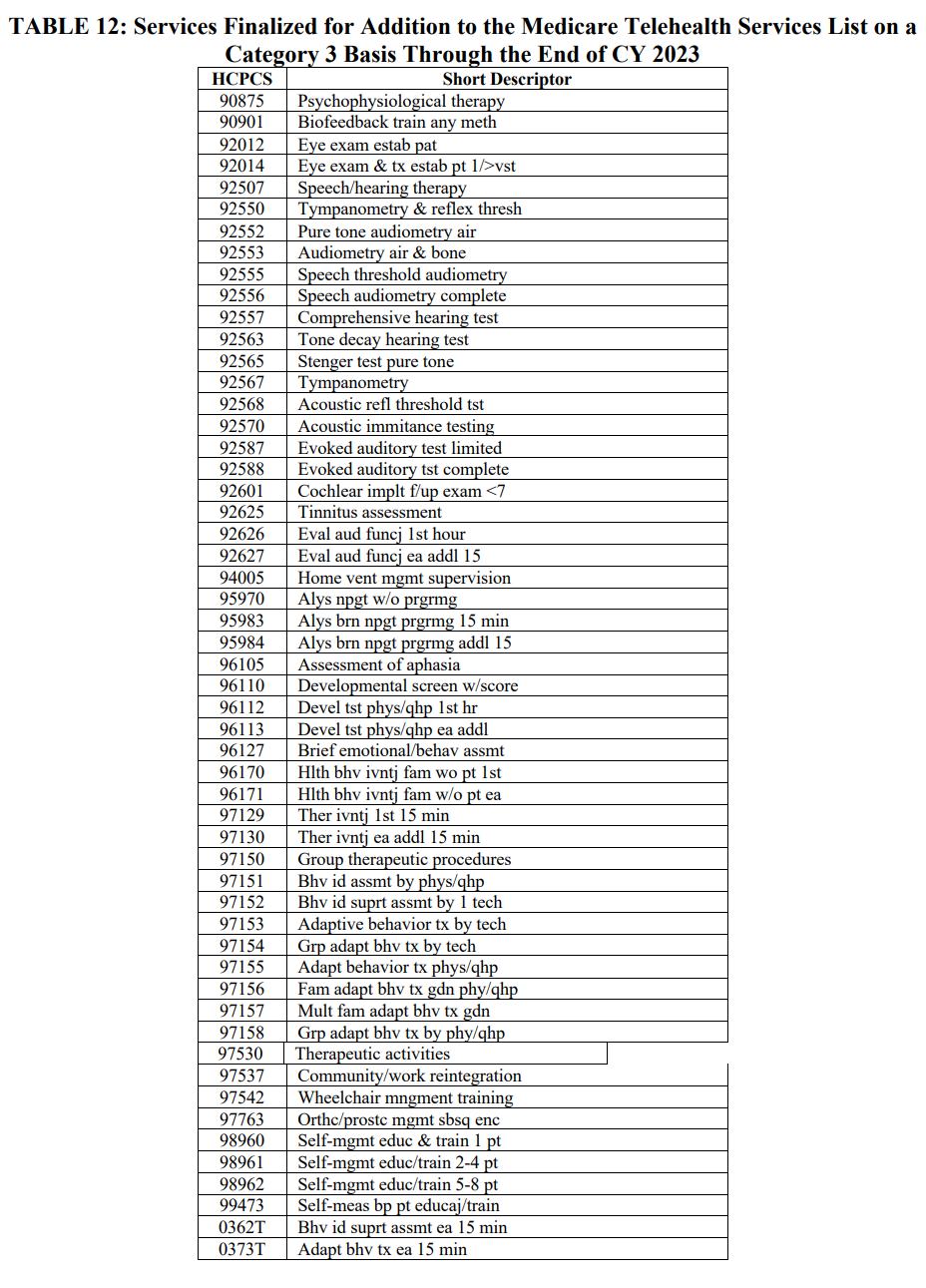
- The services added to the Medicare Telehealth Services List on a Category 3 basis includes CPT codes 90875, 92012, 92014, 92014, 92507, 94005, 96105, 96110, 96112, 96113, 96127, 96170, 96171, 97129, 97130, and 99473. (See table above)
CMS finalized its proposal to add the remote audiology testing services to the Medicare Telehealth Services List on a Category 3 basis, which would allow these services to be available via telehealth through the end of CY 2023.
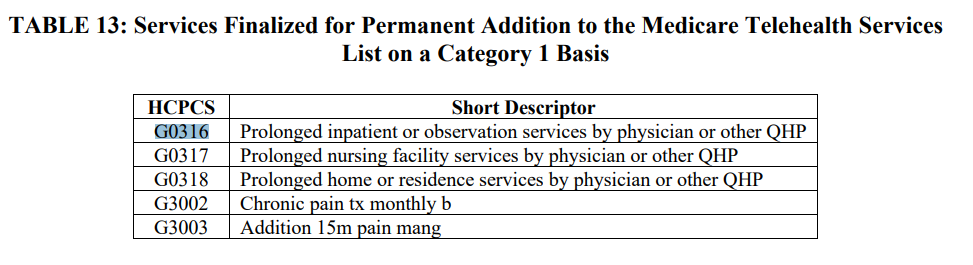
CMS finalized its proposal to create HCPCS codes G0316, G0317, G0318 to the Medicare Telehealth Services List on a Category 1 basis. These codes will be replacing existing codes that describe prolonged services, specifically inpatient prolonged services CPT codes 99356 and 99357.

Services Proposed for Removal from the Medicare Telehealth Services List After 151 Days Following the End of the PHE
As noted in the CY 2022 PFS final rule (86 FR 65054), at the conclusion of the PHE for COVID-19, the associated waivers and interim policies will expire, payment for Medicare telehealth services will once again be limited by the requirements of section 1834(m) of the Act, and CMS will return to the policies established through the regular notice-and-comment rulemaking process, through which CMS established Medicare Telehealth Services List.
CMS finalized its proposal to continue to include on the Medicare Telehealth Services List the services that are currently set to be removed from the list when the PHE ends (that is, those not currently added to the list on a Category 1, 2, or 3 basis) for an additional 151 days after the PHE ends.
Implementation of Telehealth Provisions of the Consolidation Appropriations Acts, 2021 and 2022
CMS finalized policies to implement provisions of section 1834(m) of the Act (including the amendments made by the CAA, 2021) and provisions of the CAA, 2022 that extend certain Medicare telehealth flexibilities adopted during the PHE for 151 days after the end of the PHE, including originating site, practitioner type, in-person visit requirements on mental health, and other congressionally extended authorities.
Use of Modifiers for Medicare Telehealth Services Following the End of the PHE for COVID-19
CMS finalized its proposal that Medicare telehealth services furnished on or before the 151st day after the end of the PHE, in alignment with the extensions of telehealth-related flexibilities in the CAA, 2022, will continue to be processed for payment as Medicare telehealth claims when accompanied with the modifier “95”. Practitioners will continue to bill with modifier 95 along with the POS code corresponding to where the service would have been furnished in-person through the later of the end of the year in which the PHE ends or CY 2023.
CMS finalized its proposal that, beginning January 1, 2023, a physician or other qualified health care practitioner billing for telehealth services furnished using audio-only communications technology shall append CPT modifier “93” to Medicare telehealth claims (for those services for which the use of audio-only technology is permitted under § 410.78(a)(3)), to identify them as having been furnished using audio-only technology. CMS believes that using modifier “93”, which is a CPT modifier, will simplify billing, as this modifier is used by payers outside of Medicare.
CMS is also finalizing its proposal to require all providers including RHCs, FQHCs, and OTPs to use modifier “93” when billing for eligible mental health services furnished via audio-only telecommunications technology. Providers have the option to use the “FQ” or the 93” modifiers or both where appropriate and true, since they are identical in meaning. Supervising practitioners continue to be required to append the “FR” modifier on any applicable telehealth claim when they provide direct supervision for a service using virtual presence through real-time, audio and video telecommunications technology.

Other Non-Face-to-Face Services Involving Communications Technology Under the PFS
Expiration of PHE Flexibilities for Direct Supervision Requirements
CMS changed the definition of “direct supervision” during the PHE for COVID-19 as it pertains to supervision of diagnostic tests, physicians’ services, and some hospital outpatient services, to allow the supervising professional to be immediately available through virtual presence using real-time audio/video technology, instead of requiring their physical presence.
CMS sought comment on whether the flexibility to meet the immediate availability requirement for direct supervision through the use of real-time, audio/video technology should potentially be made permanent, and on the possibility of permanently allowing immediate availability for direct supervision through virtual presence using real-time, audio/video technology for only a subset of services.
In the final rule, CMS notes that it plans to continue to gather information on this topic. CMS believes allowing additional time to collect information and evidence for direct supervision through virtual presence will help CMS to better understand the potential circumstances in which this flexibility could be appropriate permanently, outside of the PHE for COVID-19. CMS expects to continue to permit direct supervision through virtual presence through at least the end of CY 2023.
Telehealth Facility Payment Rate
CMS has abandoned its proposal to pay telehealth at the facility rate following the 151-day period. It is instead finalizing a proposal to continue to allow for payment be made for Medicare telehealth services at the rate that ordinarily would have been paid under the PFS if the services were furnished in-person, through the latter of the end of the of CY 2023 or the end of the calendar year in which the PHE ends. For those services furnished in a facility as an originating site, POS 02 may be used, and the corresponding facility fee can be billed, per pre-PHE policy, beginning the 152nd day after the end of the PHE. CMS is concerned about issues raised by commenters related to payment stability in the post-PHE period as care delivery will potentially be transitioning between virtual, hybrid, and in-person models.
Telehealth Originating Site Facility Fee Update
For CY 2023, the final payment amount for HCPCS code Q3014 (Telehealth originating site facility fee) is $28.64. The CY2022 rate was $27.59
Rural Health Clinics (RHCs) and Federally Qualified Health Centers (FQHCs)
CMS finalized the proposal to implement sections 303 and 304 of the Consolidated Appropriations Act, 2022 to:
- Temporarily continue payment for telehealth services furnished by FQHCs and RHCs for the 151-day period beginning on the first day after the end of the COVID-19 PHE using the methodology established for telehealth services furnished by FQHCs and RHCs during the PHE, which is based on payment rates that are similar to the national average payment rates for comparable telehealth services under the PFS.
- Delay the in-person requirements under Medicare for mental health services furnished through telehealth under the PFS and for mental health visits furnished by RHCs and FQHCs via telecommunications technology for a 151-day period beginning on the first day after the end of the public health emergency (PHE) for COVID-19. These proposals are necessary to fulfill these statutory requirements.
Remote Therapeutic Monitoring Services
CMS is not finalizing the proposal to create 4 new G-codes, (GRTM-1-4) which were proposed to address various issues relating to incident-to services, inclusions of clinical staff time, and supervision levels. CMS agreed that confusion remains about how the new G-codes, if finalized, would or would not possibly create a chilling effect on the availability of RTM services. CMS will continue to gather information and consider the need for further rulemaking regarding these services.
Instead, the rule, includes a clarification and new policy regarding the billing requirements for the current RTM codes: CPT codes 98975, 98976, 98977, 98980, and 98981. Beginning January 1, 2023, below modifications to our existing RTM policies take effect:
- General supervision for all RTM services- Any RTM service may be furnished under general supervision requirements.
- Cognitive behavioral therapy monitoring device – CMS is finalizing the proposal to accept the RUC recommendation to contractor price CPT code 989X6, a PE-only device code.
Behavioral Health
Tele-behavioral health
In-Person Requirement
Section 304(a) of the CAA, 2022 amended section 1834(m)(7)(B)(i) of the Act to delay the requirement for an in-person visit with a physician or practitioner within 6 months prior to an initial mental health telehealth service, and again at subsequent intervals as the Secretary determines appropriate. In light of this amendment, the in-person requirements for telehealth services furnished for purposes of diagnosis, evaluation, or treatment of a mental health disorder will again be effective on the 152nd day after the PHE ends. In addition, section 304(b) and (c) of the CAA, 2022 modified sections 1834(y) and 1834(o)(4) of the Act, respectively, to similarly delay in-person visit requirements for mental health visits furnished by Rural Health Clinics and Federally Qualified Health Centers via telecommunications technology.
CMS clarifies in the final rule that CMS does not believe the in-person requirement applies to beneficiaries who began receiving mental health telehealth services in their homes during the PHE. In other words, if a beneficiary began receiving mental health telehealth services during the PHE or during the 151-day period after the end of the PHE, then they would not be required to have an in-person visit within 6 months; rather, they will be considered established and will instead be required to have at least one in-person visit every 12 months (so long as any such subsequent telehealth service is furnished by the same individual physician or practitioner (or a practitioner of the same sub-specialty in the same practice) to the same beneficiary). This means that these services would be subject to the requirement that an in-person visit is furnished within 12 months of each mental health telehealth service for those services that are subject to in-person visit requirements (unless an exception is documented by their treating practitioner).
Chronic Pain Management and Treatment (CPM) Bundles (HCPCS GYYY1, and GYYY2)
In the CY 2022 PFS proposed rule (86 FR 39104, 39179 – 39181), CMS explored refinements to the PFS that would appropriately value chronic pain management and treatment (CPM) by soliciting comment on CPM for the purpose of future rulemaking. In CMS’s solicitation, they described Federal efforts for more than a decade to effectively address pain management as a response to the nation’s overdose crisis, such as the National Pain Strategy and the HHS Pain Management Best Practices Inter-Agency Task Force Report.
Through solicitation of comments, the CCM/CCCM/PCM code family now includes five sets of codes, each set with a base code and an add-on code. The sets vary by the degree of complexity of care, who directly performs the services, and the time spent furnishing the services. The RUC-recommended values for work RVUs and direct PE inputs for these codes in CY 2022 were derived from a recent RUC specialty society survey.
CMS has finalized its proposal to create separate coding and payment for CPM services beginning January 1, 2023.
- HCPCS Code G3002: Chronic pain management and treatment, monthly bundle including, diagnosis; assessment and monitoring; administration of a validated pain rating scale or tool; the development, implementation, revision, and/or maintenance of a person-centered care plan that includes strengths, goals, clinical needs, and desired outcomes; overall treatment management; facilitation and coordination of any necessary behavioral health treatment; medication management; pain and health literacy counseling; any necessary chronic pain related crisis care; and ongoing communication and care coordination between relevant practitioners furnishing care, e.g. physical therapy and occupational therapy, and community-based care, as appropriate. Required initial face-to-face visit at least 30 minutes provided by a physician or other qualified health professional; first 30 minutes personally provided by physician or other qualified health care professional, per calendar month. (When using G3002, 30 minutes must be met or exceeded.)
- HCPCS code G3003: Each additional 15 minutes of chronic pain management and treatment by a physician or other qualified health care professional, per calendar month. (List separately in addition to code for G3002. When using G3003, 15 minutes must be met or exceeded.)
Revisions to “Incident To” Physicians’ Services Regulation for Behavioral Health Services
In the CY 2014 PFS final rule, CMS created an exception to its “incident to” regulation under which “incident to” services generally must be furnished under direct supervision, to allow general, rather than direct, supervision when chronic care management services are furnished incident to the billing physician’s or NPP’s services outside of the practice’s normal business hours by clinical staff. In the CY2017 PFS final rule, CMS also revised regulations to allow general, rather than direct, level of supervision for designated care management services, and established that it would designate care management services through notice and comment rulemaking.
CMS noted in the proposed rule that currently there is no separate benefit category under the statute that recognizes the professional services of licensed professional counselors (LPCs) and Licensed Marriage and Family Therapists (LMFTs). Therefore, payment for the services of LPCs and LMFTs can only be made under the PFS indirectly when an LPC or LMFT performs services as auxiliary personnel incident to, the services, and under the direct supervision, of the billing physician or other practitioner.
Given CMS’ goal in the 2022 CMS Behavioral Health Strategy to improve access to and quality of mental health care services, CMS finalizes several regulatory changes to make greater use of the services of LPCs and LMFTs. CMS notes that it does not have authority to create a statutory benefit category for practitioner types, but it finalizes its proposal to amend the direct supervision requirement under the “incident to” regulation to allow behavioral health services to be furnished under the general supervision of a physician or NPP when these services or supplies are provided by auxiliary personnel incident to the services of a physician or NPP.
CMS further clarifies that any service furnished primarily for the diagnosis and treatment of a mental health or SUD can be furnished by auxiliary personnel under the general supervision of a physician or NPP who is authorized to furnish and bill for the services provided incident to their own professional services.
CMS further plans to address payment for new codes that describe caregiver behavioral management training in the CY 2024 PFS.
New Coding and Payment for General Behavioral Health Integration (BHI) billed by Clinical Psychologists (CPs) and Clinical Social Workers (CSWs)
In the CY2017 and CY2018 PFS final rules, CMS established codes and payment for monthly services furnished using the Psychiatric Collaborative Care Model (CoCM), an evidence-based approach to behavioral health integration that enhances “usual” primary care by adding care management support and regular psychiatric inter-specialty consultation, and for services furnished using other models of BHI in the primary care setting.
In those rules, CMS additionally sought comment on the circumstances under which this model of care is happening and whether additional coding would be needed to accurately describe and value other models of care. CMS received feedback that initiating visit services for BHI should include in-depth psychological evaluations delivered by a CP, and that CMS should consider allowing professionals who were not eligible to report the approved initiating visit codes to Medicare to serve as a primary hub for BHI services.
CMS is now finalizing a proposal to create a new G code describing General BHI performed by CPs or CSWs to account for monthly care integration where the mental health services furnished by a CP or CSW are serving as the focal point of care integration. The finalized new code is :
- G0323 (Care management services for behavioral health conditions, at least 20 minutes of clinical psychologist or clinical social worker time, per calendar month, with the following required elements: initial assessment or follow-up monitoring, including the use of applicable validated rating scales; behavioral health care planning in relation to behavioral/psychiatric health problems, including revision for patients who are not progressing or whose status changes; facilitating and coordinating treatment such as psychotherapy, coordination with and/or referral to physicians and practitioners who are authorized by Medicare law to prescribe medications and furnish E/M services, counseling and/or psychiatric consultation; and continuity of care with a designated member of the care team.)
CMS has finalized its proposal to value this service under the proposed HCPCS code G0323 based on a direct crosswalk to the work values and direct PE inputs for CPT code 99484 (Care management services for behavioral health conditions, at least 20 minutes of clinical staff time, directed by a physician or other qualified health care professional, per calendar month, with the following required elements: initial assessment or follow-up monitoring, including the use of applicable validated rating scales; behavioral health care planning in relation to behavioral/psychiatric health problems, including revision for patients who are not progressing or whose status changes; facilitating and coordinating treatment such as psychotherapy, pharmacotherapy, counseling and/or psychiatric consultation; and continuity of care with a designated member of the care team), because the services described by GBHI1 closely mirror those described by CPT code 99484.
Modifications Related to Medicare Coverage for Opioid Use Disorder (OUD) Treatment Services Furnished by Opioid Treatment Programs (OTPs)
Section 2005 of the Substance Use-Disorder Prevention that Promotes Opioid Recovery and Treatment for Patients and Communities (SUPPORT) Act established a new Medicare Part B benefit category for OUD treatment services furnished by OTPs during an episode of care beginning on or after January 1, 2020. CMS implemented Medicare coverage and provider enrollment requirements and established a methodology for determining the bundled payments for episodes of care for the treatment of OUD furnished by OTPs, among other related policies, in the CY2020 PFS final rule. CMS subsequently adopted new add-on codes and payment, and made certain policy changes, in the CY2021 and CY2022 final rules.
CMS has now finalized several additional updates to payment and policies regarding OUD treatment services furnished by OTPs.
- Methadone Pricing – CMS has finalized its revised methodology for pricing the drug component of the methadone weekly bundle and the add-on code for take-home supplies of methadone. CMS will base the payment amount for the drug component of HCPCS codes G2067 and G2078 for CY 2023 and subsequent years on the payment amount for methadone in CY 2021 and update this amount annually to account for inflation using the PPI for Pharmaceuticals for Human Use (Prescription).
- Proposed Changes to the Rate for Individual Therapy in the Bundled Rate – CMS has finalized its proposal to modify the payment rate for the non-drug component of the bundled payments for episodes of care to base the rate for individual therapy on a crosswalk code describing a 45-minute session, rather than the current crosswalk to a code describing a 30-minute session.
- Mobile Components Operated by OTPs – CMS clarifies that OTPs can bill Medicare for medically reasonable and necessary services furnished via mobile units in accordance with SAMHSA and DEA guidance. CMS finalizes its proposal that locality adjustments for services furnished via mobile units would be applied as if the service were furnished at the physical location of the OTP registered with DEA and certified by SAMHSA.
- Flexibilities for OTPs to Use Telecommunications for Initiation of Treatment with Buprenorphine – CMS has finalized its proposal to allow the OTP intake add-on code to be furnished via two-way audio-video communications technology when billed for the initiation of treatment with buprenorphine, to the extent that the use of audio-video telecommunications technology to initiate treatment with buprenorphine is authorized by DEA and SAMHSA at the time the service is furnished. CMS also finalizes its proposal to permit the use of audio-only communication technology to initiate treatment with buprenorphine in cases where audio-video technology is not available to the beneficiary.
Comment Solicitation on Intensive Outpatient Mental Health Treatment, including Substance Use Disorder (SUD) Treatment, Furnished by Intensive Outpatient Programs (IOPs)
CMS noted in the proposed rule that there are a range of services described by existing coding under the PFS that can be billed for treatment of mental health conditions, including SUDs, such as individual, group, and family psychotherapy. Over the past several years, CMS has increased the coding and payment mechanisms for substance use treatment services paid under the PFS.
CMS requested feedback on whether the current coding and payment mechanisms under the PFS adequately account for intensive outpatient services that are part of a continuum of care in the treatment, among other information.
CMS thanks commenters for their feedback and may consider the comments in future rulemaking.
Comment Solicitation on Payment for Behavioral Health Services under the PFS
CMS solicited comment on how it can best ensure beneficiary access to behavioral health services, including any potential adjustments to the PFS rate-setting methodology, for example, any adjustments to systematically address the impact on behavioral health services paid under the PFS.
CMS noted that it appreciates the feedback received and may consider the comments in future rulemaking.